Japanese encephalitis information for vets – pigs
Japanese encephalitis is a mosquito-borne viral disease that can cause reproductive losses in pigs, and encephalitis in horses and very rarely in other species. Other animals do not usually show any signs, and pigs and horses may often show no signs at all. It is caused by Japanese encephalitis virus which is a member of the Flavivirus genus. In infected human around 1% will develop clinical disease.
Japanese encephalitis was first detected in Victoria in February 2022, with pig cases, human cases and evidence of some horses being exposed to the virus.
In the 2021-22 summer, the disease was reported on 23 pig farms in northern Victoria. No cases were reported In the 2022-23 summer, even through the seasonal conditions appeared to be favourable. It is hard to predict if the disease will reappear in the 2023-24 season.
The disease remains on the notifiable list in Victoria, where is it no longer considered exotic, but seasonally, sporadically endemic.
If you suspect Japanese encephalitis in any animal phone the all-hours - Emergency Animal Disease Hotline on 1800 675 888.
Information for Veterinarians for pigs
Japanese encephalitis (JE) is a mosquito-borne viral disease that can cause reproductive losses and encephalitis in susceptible animal species. It is caused by Japanese encephalitis virus which is a member of the Flavivirus genus.
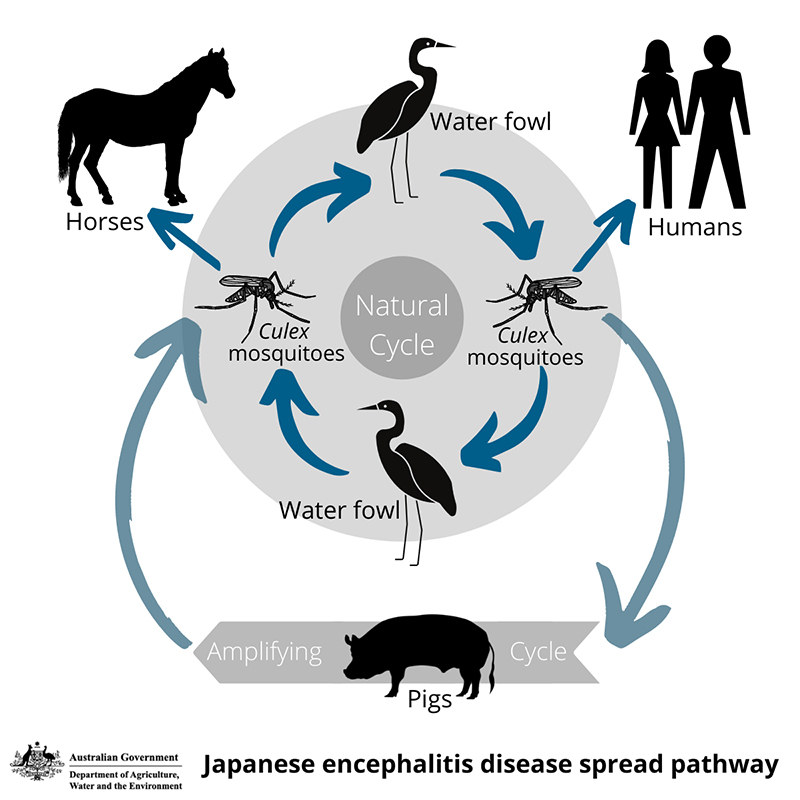
The virus is primarily spread by mosquitoes feeding on infected animals and does not usually spread directly from animal to animal (i.e. it is not considered contagious). Certain types of mosquitoes, such as Culex sp. can become infected with JE virus and these tend to be most active at dawn and dusk.
Infected pigs do not transmit the infection to other animals but may infect mosquitoes if bitten while they still have the virus in their blood.
Other livestock such as horses, cattle, sheep and goats are ‘dead end’ hosts and cannot transmit the disease back to mosquitoes.
In general, spread of the virus is through the movement of infected mosquitoes, often over long distances due to wind dispersal and the movement of herons and egrets. Herons and egrets can carry the virus but are not affected by it.
In pigs the most common clinical signs are mummified and stillborn or weak piglets, some with neurological signs. Other farms have seen overterm litters being born where some of the piglets have no brains. In a previously uninfected population, litters from sows and gilts are expected to be equally affected. Adult sows and piglets infected post-birth do not show overt signs of disease and appear quite healthy. Boars, if present on farm, may experience fever, infertility and oedematous testicles.
In horses many cases are asymptomatic and most clinical disease is mild, however more severe encephalitis can occur which can be fatal. Signs include fever, lethargy, anorexia and neurological signs which vary with severity of the clinical disease. Neurological signs can include incoordination, difficulty swallowing, impaired vision, and rarely a hyperexcitable form occurs. Disease has also been reported in donkeys and one alpaca was confirmed with the disease in South Australia during the 2022 outbreak.
What should be collected in the field?
Post-mortem samples from deceased (<12 hours) and euthanased piglets from affected litters
Necropsy three (3) aborted / stillborn / neonatal piglets
- Fresh samples (or frozen) of cerebral cortex or CSF if no tissue, placenta in individual containers, plus another container of pooled tissues from the spleen, heart, lung, liver and kidney.
- Fixed samples from one (1) piglet (i.e. not from mummified foetuses): brain, cervical spinal cord, lung, heart, liver, kidney and placenta.
Undertake the investigation, complete the RODE forms (PDF - 384.1 KB) as described and follow the sample submission guidelines in the Significant Disease Investigation Guide – Pigs
Download:
- Significant Disease Investigation Guide - Pigs (PDF - 897.7 KB)
- Significant Disease Investigation Guide - Pigs- accessible (WORD - 900.0 KB)
Be aware of this and other potential zoonoses – collect samples carefully and wear appropriate PPE including gloves, eye protection and a mask. The danger during sample collection is from splash or stick injuries.
Submitting samples and reports
Veterinary Diagnostic Services
AgriBio Specimen reception
Main loading dock
5 Ring Rd
La Trobe University
Bundoora 3083
Phone: (03) 9032 7515
Email: vet.diagnostics@agriculture.vic.gov.au.
The samples will undergo a suite of triage tests that are targeting Flavivirus. This will take about three days.
If the samples return a negative result at this initial stage, you will be contacted by Agriculture Victoria staff.
Positive samples may go to the CSIRO Australian Centre for Disease Preparedness for further testing which may take several weeks.
There are two ways to protect yourself: avoiding mosquito bites and vaccination.
The Department of Health recommends people protect themselves and their families against mosquito-borne diseases:
- Wear long, loose fitting clothes outdoors.
- Use effective mosquito repellents containing picaridin or DEET on all exposed skin.
- Try to limit outdoor activity if lots of mosquitoes are about.
- Use ‘knockdown’ fly sprays and plug-in repellent devices indoors.
- Sleep under mosquito nets treated with insecticides if you don’t have flywire screens on windows on your home or are sleeping in an untreated tent or out in the open.
- Mosquito coils can be effective in small outdoor areas where you gather to sit or eat.
- Remove mosquito breeding sites like stagnant water around your property.
A small number of people infected with JE virus may become seriously ill with encephalitis (inflammation of the brain). Other people may develop an illness with fevers, headaches and aches and pains.
Symptoms of encephalitis may include rapid onset of fever, headache, sensitivity to light, neck stiffness, vomiting, confusion or disorientation and sometimes seizures, progressing to coma. Anyone experiencing symptoms, particularly if they’ve visited regions near the border of Victoria and New South Wales or been in contact with pigs or with mosquitoes should seek urgent medical attention.
Any person who has been in contact with pigs and is experiencing any of the symptoms should seek urgent medical attention. Further information can be found on the Better Health website.
Vaccines for horses and pigs are used in some countries where the disease is endemic. No vaccines for animals are registered for use in Australia. The issues around vaccination of livestock are under consideration.
The movement of livestock, livestock semen, pig feed and human movements will not be restricted.
Download the Information for Veterinarians for pigs (PDF - 266.4 KB)